
No more pain in the neck: Disc replacement procedure offers Linda lasting relief
Linda Horne thought she had strained a muscle at first.
But the minor twinge that started after one of her regular weight-lifting sessions soon grew into intense shoulder pain with accompanying arm and wrist weakness that threatened to sidetrack her busy life.
She had a ruptured disc in her cervical (neck) spine.
“It completely changed my life as I had known it,” Horne says.
Luckily, she found WashU Medicine spinal surgeon Jacob Buchowski, MD, of the Spine and Joint Center at Barnes-Jewish West County Hospital. Dr. Buchowski performed a procedure that returned Horne to her normal life within weeks.
The procedure — cervical disc replacement — is an option for certain patients, like Linda Horne, whose specific injury type and location make them good candidates, says Dr. Buchowski. Its advantages include a less invasive operation, faster recovery and reduced chance of further degeneration compared to the disc fusion surgery typically performed, he says.
Horne, 61, a psychiatrist who lives and works in Clayton, was active, walking to and from work daily, in addition to working out regularly.
Then came the nagging pain in her lower neck, upper back, and trapezial (shoulder blade) area. Often, spinal injuries can be managed by simply taking anti-inflammatories and resting or cutting back on exercise as the injury heals, says Dr. Buchowski. But Horne’s pain continued to worsen and made normal daily activities exhausting.
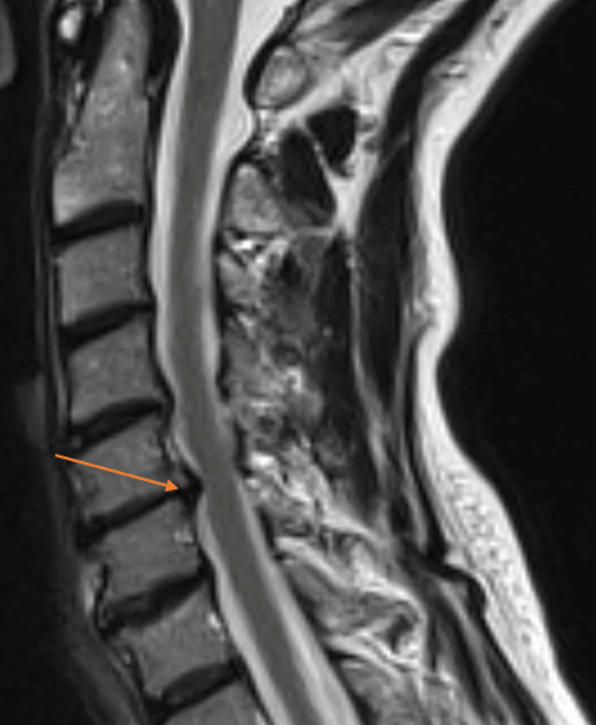
MRI image of ruptured disc in Linda’s neck.
Typically, after seeing patients all day, she’d walk home from her office, cook dinner for her husband and herself and stay busy with home or art projects. Instead, Horne would come home and crawl into bed.
“My life as I had known it went away,” she says. “I couldn’t sit all day in that kind of pain.”
Even more worrisome, Horne developed tingling and numbness in her hand and weakness in her arm and wrist, indicating nerve damage. Trigger point injections and steroids didn’t help.
A magnetic resonance image (MRI) confirmed that the disc between the C5 and C6 vertebrae in Horne’s neck had ruptured and was pressing on surrounding nerves, causing the weakness and pain. It also showed mild arthritic changes in her spine contributing to the nerve compression.
One of her husband’s colleagues at Washington University suggested that Horne see Dr. Buchowski.
Cervical Disc Replacement Surgery Relieves Pain
Dr. Buchowski met with Horne and reviewed her imaging. Given her unrelenting pain and development of upper extremity weakness and numbness, he told her that surgery was her best option for relieving her symptoms and preventing further nerve damage.
For many patients with similar conditions, surgery would involve removing the damaged disc between the two vertebrae, then fusing the vertebrae together with a bone graft and metal rods or plates.
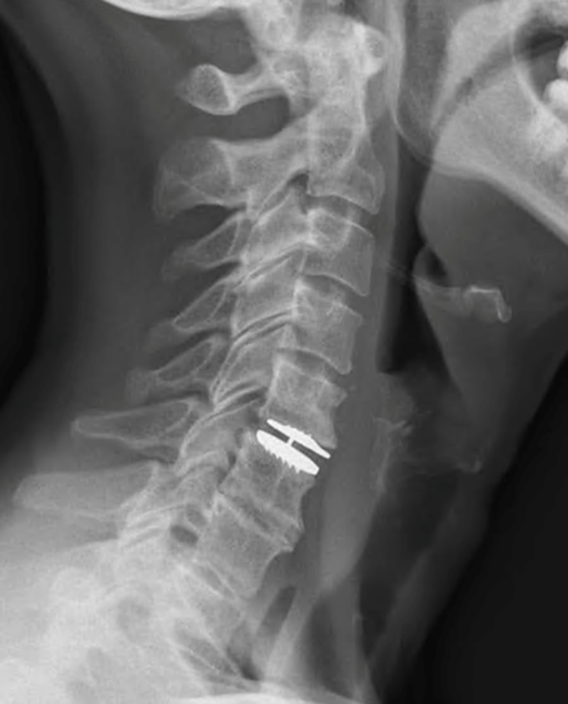
MRI image after disc replacement surgery.
While spinal fusion surgery has long been an accepted treatment for many patients, it has some drawbacks — including some loss of mobility in the neck, placing increased stress on the adjacent discs, and potentially an increased chance of developing degenerative changes at the levels adjacent to the fused level — leading to what is called adjacent segment disease, says Dr. Buchowski.
Instead, Horne and Dr. Buchowski agreed that given her relative lack of neck pain and her normal motion at the disc level resulting in her symptoms, cervical disc replacement surgery would be her best option. The procedure would minimize the extent of surgery required while relieving the pressure on the affected nerves and preserving motion.
Cervical disc replacement involves removing the damaged disc through a small incision in the front of the neck and replacing it with an artificial disc. Patients usually retain full mobility in their neck and recovery is generally quick, allowing patients to return to work within several weeks of the procedure.
Although most patients undergoing this procedure are age 50 or younger, Horne’s excellent health and physical condition made her a good candidate for the surgery, Dr. Buchowski says.
Horne had outpatient disc replacement surgery at Barnes-Jewish West County Hospital in early November 2020 and was home within several hours of the procedure.
Her recovery was smooth from the start, she says. When she awoke after surgery, the intense shoulder pain was gone. And other than some mild muscle stiffness and hoarseness, she had no major side effects.
Back to Strength Training
Now, almost a year after the surgery, mild residual weakness in one arm and wrist is the only remnant of her ordeal. She’s returned to her regular exercise and even Pilates and weightlifting.
“It’s a marvelous procedure,” Horne says. “Disc replacement is a wonderful example of the great advances in spine surgery. I have my life back. I am so grateful.”